NABH Maturity & Digital Standards (Speaker: Mr. Avinash Pandey)
🏛 Constellations — Institutional NABH Maturity, Governance & Resource Challenges.
Institutional Standards: NABH & The Maturity Path (Speaker: Mr. Avinash Pandey)
Section titled “Institutional Standards: NABH & The Maturity Path (Speaker: Mr. Avinash Pandey)” Figure: The National Digital Health Mission ecosystem, creating a unified pathway for patient safety and interoperability.
Figure: The National Digital Health Mission ecosystem, creating a unified pathway for patient safety and interoperability.
JCI vs. NABH: A Global-Local Bridge
Section titled “JCI vs. NABH: A Global-Local Bridge”A common question arises regarding the choice between international and national standards. While JCI (Joint Commission International) is a prestigious global benchmark, it is primarily designed for western, developed contexts where patient quality awareness and secondary infrastructure are already at a high baseline.
- The India Reality: India requires a Tiered Approach. NABH standards are explicitly designed to account for varying institutional strength, digital maturity, and geographic location (Tier 1 vs. Tier 2/3).
- Progressive Maturity: Instead of a “pass-fail” global hurdle, NABH allows hospitals to grow through tiered accreditation, making quality excellence achievable for everyone from a rural 30-bed hospital to a metropolitan multi-specialty center.
The 8-Chapter Modular Framework (NABH DHS)
Section titled “The 8-Chapter Modular Framework (NABH DHS)”To ensure structured and progressive growth, the NABH Digital Health Standards (DHS) are organized into 8 key chapters, bifurcated into Clinical and Non-clinical domains. This framework comprises 38 Standards and 182 Objective Elements.
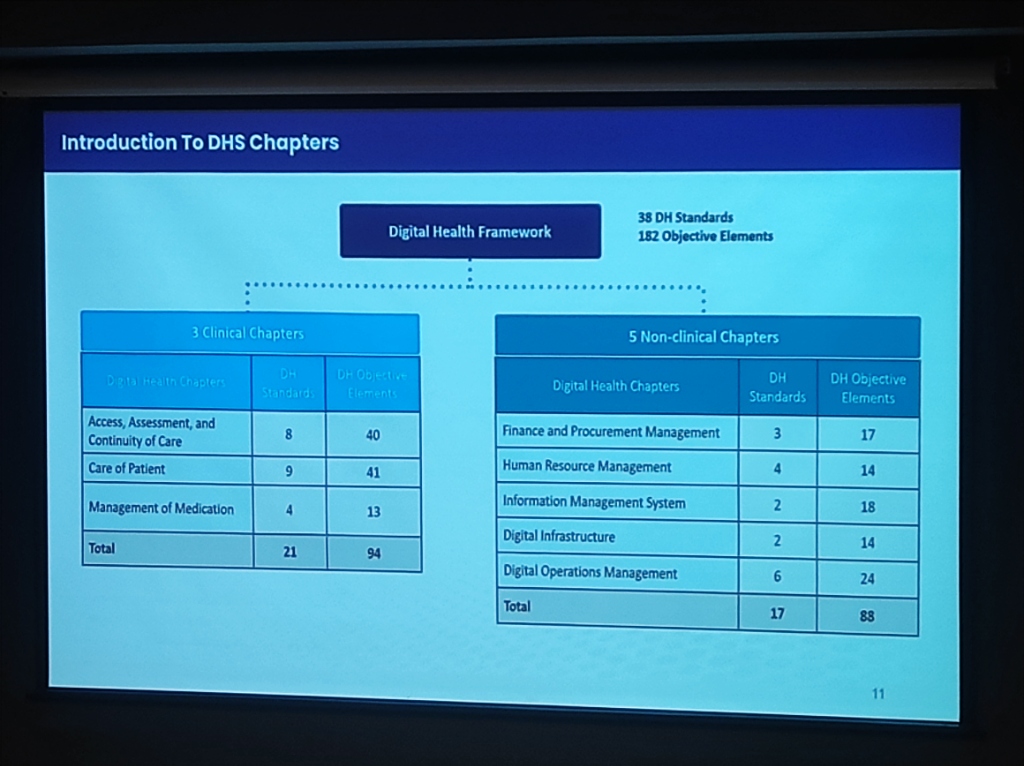 Figure: The structural breakdown of NABH Digital Health Standards—Clinical vs. Non-Clinical chapters.
Figure: The structural breakdown of NABH Digital Health Standards—Clinical vs. Non-Clinical chapters.
| Digital Health Chapter | Standards | Objective Elements |
|---|---|---|
| 3 Clinical Chapters | 21 | 94 |
| Access, Assessment, and Continuity of Care (AAC) | 8 | 40 |
| Care of Patients (COP) | 9 | 41 |
| Management of Medication (MOM) | 4 | 13 |
| 5 Non-Clinical Chapters | 17 | 88 |
| Finance and Procurement Management | 3 | 17 |
| Human Resource Management | 4 | 14 |
| Information Management System (IMS) | 2 | 18 |
| Digital Infrastructure | 2 | 14 |
| Digital Operations Management | 6 | 24 |
| Total | 38 | 182 |
Breaking the Silos: A Unified Mission
Section titled “Breaking the Silos: A Unified Mission”As Avinash Pandey highlights, one of the greatest contributions of NABH digital standards is their ability to break organizational silos.
- The Trinity of Adoption: Successful EMR adoption is no longer just an “IT project.” It is a unified mission where the Clinical, Quality, and IT teams come together.
- Standardized Quality: Quality teams provide the data integrity benchmarks, clinical teams provide the operational reality, and IT teams provide the technical backbone. This cross-functional collaboration is the key to moving from fragmented data to a cohesive digital health ecosystem.
Small-Hospital Scalability: Design for India’s Reality
Section titled “Small-Hospital Scalability: Design for India’s Reality”A common misconception is that digital standards are only for large corporate hospitals. On the contrary, NABH standards are explicitly designed to be inclusive of 30-50 bed hospitals, which form the backbone of Indian healthcare.
- Remote Adoption: Small hospitals in remote regions—from Manipur to Jammu & Kashmir—are already adopting these standards, proving that digital maturity is a function of leadership more than bed count.
Lightweight EMR Strategies: Pragmatic Digital Adoption
Section titled “Lightweight EMR Strategies: Pragmatic Digital Adoption”One of the most significant insights from the current national rollout is that Small and Medium healthcare facilities need not have a full-fledged, complex EMR to participate in the digital ecosystem.
- Micro-EMR Solutions: The NHA is actively collaborating with and promoting lightweight platforms like eSushrut and eKa Care. These solutions provide the core digital building blocks (ABHA linkage, consultation logging, and report sharing) without the overhead and cost of a Tier-1 enterprise system.
- Modular Growth: This strategy allows smaller clinics and nursing homes to achieve basic digital compliance almost immediately, with the path to add more complex clinical modules as they scale or their needs evolve.
- Democratizing Quality: By lowering the entry barrier, even a small community hospital can achieve the same data integrity and patient safety benchmarks as a Tier-1 institution.
The ROI of Standards: Measurable Impact
Section titled “The ROI of Standards: Measurable Impact”Standards are not just about compliance; they are a direct driver of institutional revenue and operational velocity. Hospitals adopting high-quality digital health standards report significant improvements across clinical and administrative KPIs:
 Figure: Measurable KPI improvements reported by hospitals adopting national digital health standards.
Figure: Measurable KPI improvements reported by hospitals adopting national digital health standards.
- Operational Velocity:
- 30% Reduction in Patient Waiting Time: Dramatically increasing patient volume and clinic efficiency.
- 20% Reduction in Discharge TAT: Faster bed turnover, allowing for more revenue-generating admissions.
- 39% Diagnostic TAT Reduction: Ensuring faster delivery of diagnostic reports for quicker clinical decisions.
- Revenue & Efficiency:
- 18% Reduction in Prescription Bounces: Direct revenue growth for hospital pharmacies.
- 15% Blood Component TAT Reduction: Faster delivery of critical blood components.
- Patient Safety & Accuracy:
- 10% Medication Accuracy Improvement: Improvement in accuracy during medication administration.
- 100% Patient Record Access: Achieving full access to patient records from past and current visits.
Integrated & Simplified Approach
Section titled “Integrated & Simplified Approach”India is pioneering a simplified approach to digital health standards through an integrated “A-B-C” framework. This ensures that technical certification at the vendor level directly enables institutional compliance at the hospital level.
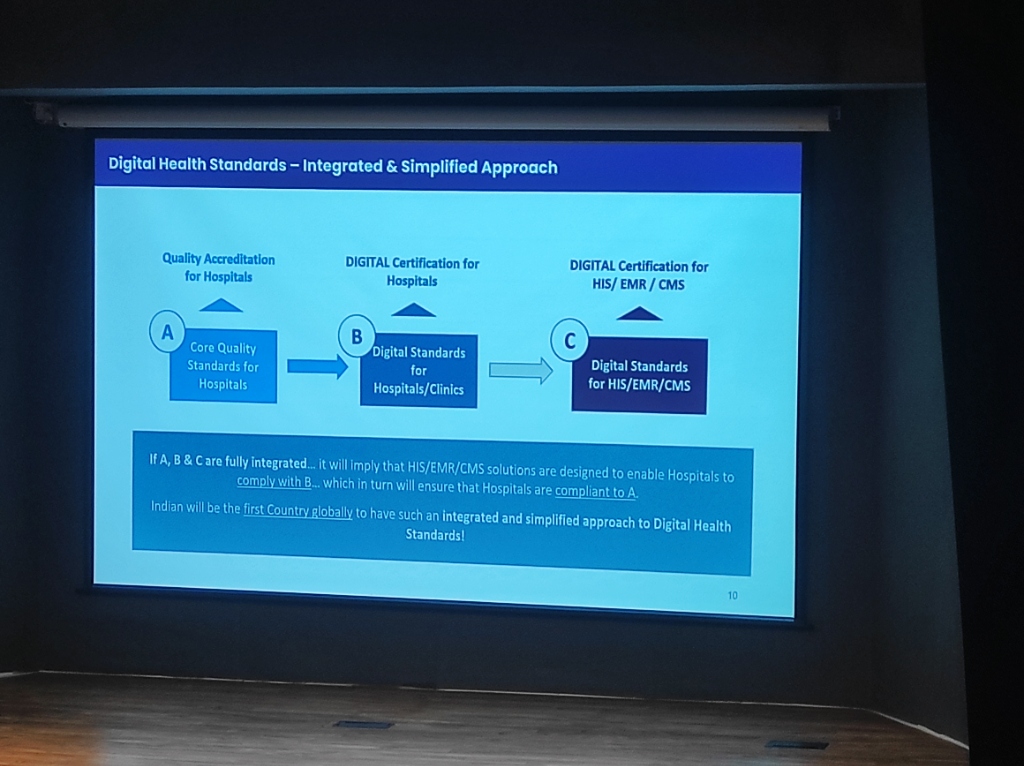 Figure: The integrated approach connecting Quality Accreditation (A), Hospital Digital Certification (B), and System Digital Certification (C).
Figure: The integrated approach connecting Quality Accreditation (A), Hospital Digital Certification (B), and System Digital Certification (C).
- (A) Quality Accreditation for Hospitals: Core quality benchmarks for patient care.
- (B) Digital Standards for Hospitals/Clinics: Ensuring the institution follows digital best practices.
- (C) Digital Standards for HIS/EMR/CMS: Technical standards that software vendors must meet.
The Integration Logic: If A, B, and C are fully integrated, it implies that HIS/EMR/CMS solutions are designed to enable Hospitals to comply with Digital Standards (B), which in turn ensures that Hospitals are compliant with overall Quality Accreditation (A).
The Certification Shortcut
Section titled “The Certification Shortcut”For hospitals looking to accelerate their accreditation, NABH has simplified the compliance burden. Institutions that adopt Digital Certified HIS, EMR, or Practice Management Systems (PMS) automatically ensure a large part of their clinical and operational compliance.
However, a critical distinction exists between Certification and Operational Impact:
- The M1/M2/M3 Gap: While many systems are certified for Milestones (M1/M2/M3), the actual implementation often falls into the “Photo-Upload” Trap. Instead of capturing structured, clinical-grade data, some implementers simply upload photos of paper records to meet compliance.
- Structured Data for AI: This shortcut renders the data useless for AI-driven clinical decision support. True impact requires native structured data entry at the point of care, moving beyond simple digitization of paper.
